Lactose intolerance affects millions of people worldwide, yet many remain unaware they have it. Unlike a milk allergy, which involves the immune system, lactose intolerance stems from the digestive system’s inability to fully break down lactose—the natural sugar found in milk and dairy products. Symptoms can range from mild discomfort to disruptive gastrointestinal issues. Recognizing the signs early and confirming them through reliable methods can help you make informed dietary choices and improve your quality of life.
Understanding Lactose Intolerance
Lactose is broken down in the small intestine by an enzyme called lactase. When lactase production declines—either due to genetics, aging, or intestinal damage—undigested lactose moves into the colon, where bacteria ferment it. This fermentation process produces gas and draws water into the bowel, leading to the hallmark symptoms of lactose intolerance.
There are three main types:
- Primary lactose intolerance: The most common form, caused by a natural decline in lactase after childhood, especially prevalent in people of Asian, African, Hispanic, and Mediterranean descent.
- Secondary lactose intolerance: Results from injury to the small intestine due to illness, surgery, or conditions like celiac disease or Crohn’s disease.
- Congenital or developmental: Rare, present from birth, where infants produce little or no lactase.
“Lactose intolerance isn’t dangerous, but ignoring it can lead to chronic discomfort and unnecessary distress. Proper identification allows for effective management.” — Dr. Rachel Nguyen, Gastroenterologist
Key Signs of Lactose Intolerance
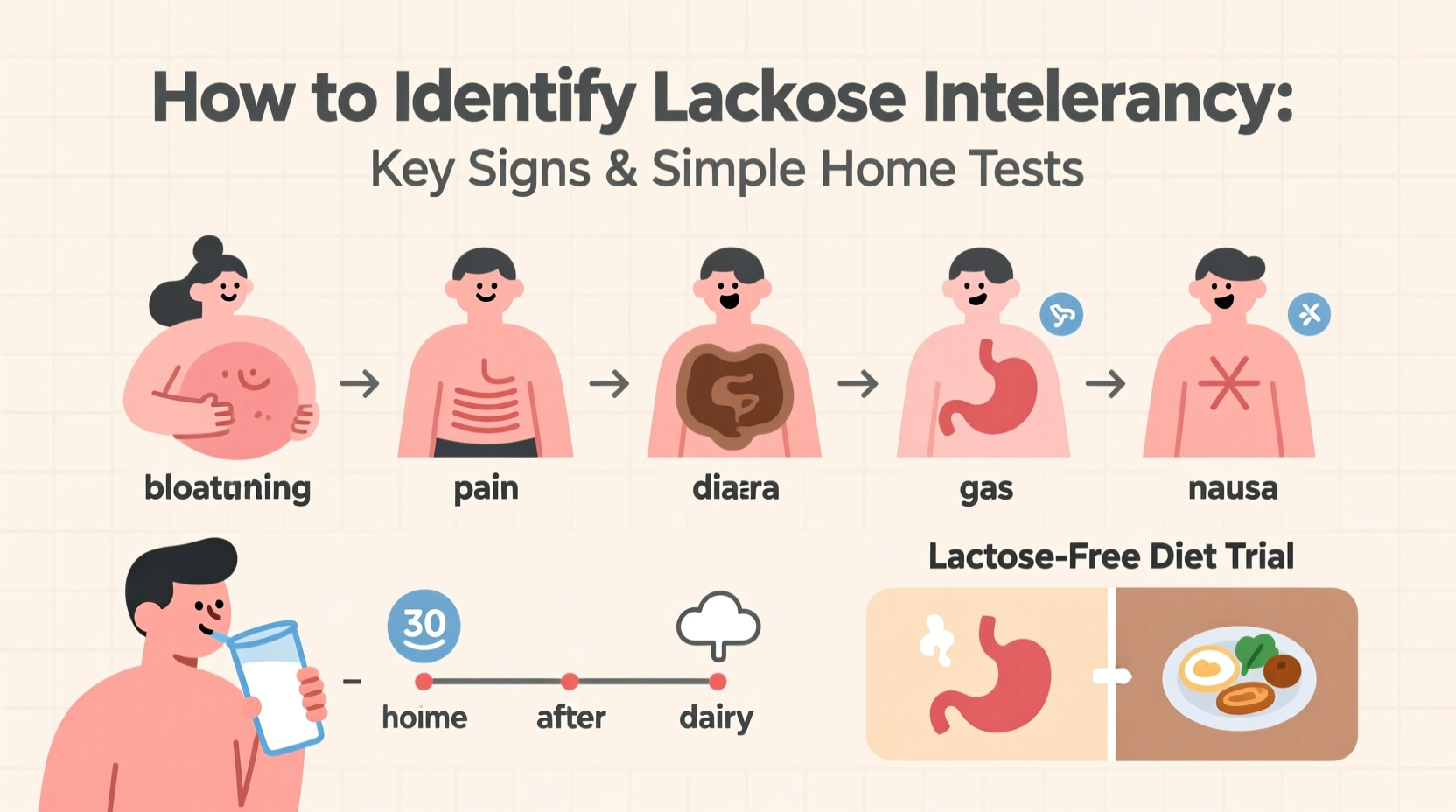
Symptoms typically appear 30 minutes to two hours after consuming dairy and vary in intensity based on the amount of lactose ingested and individual tolerance levels. Common signs include:
- Bloating and abdominal distension
- Gas (flatulence)
- Abdominal cramps or pain
- Diarrhea, often watery and urgent
- Nausea, sometimes with vomiting
- Gurgling or rumbling sounds in the lower abdomen
It's important to note that these symptoms overlap with other digestive disorders such as irritable bowel syndrome (IBS), milk protein allergy, or small intestinal bacterial overgrowth (SIBO). Therefore, symptom tracking and testing are essential for accurate self-assessment.
Simple Home Tests You Can Try
While medical tests like the hydrogen breath test or lactose tolerance blood test offer definitive diagnoses, several safe and practical home-based approaches can provide strong preliminary evidence.
1. Elimination Diet Trial
This is the most reliable method for self-testing. Remove all lactose-containing foods from your diet for 2–3 weeks. If symptoms resolve, reintroduce a controlled amount of lactose (e.g., a glass of milk) and monitor your body’s response.
- Phase 1: Eliminate all dairy (milk, cheese, yogurt, butter, cream, whey, casein).
- Phase 2: After 14 days without symptoms, drink 8 oz of regular milk on an empty stomach.
- Phase 3: Observe for symptoms over the next 48 hours.
If symptoms return after reintroduction, lactose intolerance is likely.
2. Milk Challenge Test
A quicker version of the elimination trial. After going dairy-free for a few days, consume 250ml of whole milk first thing in the morning. Avoid eating anything else for 3–4 hours. If bloating, gas, or diarrhea develops within two hours, it may indicate poor lactose digestion.
3. Lactose-Free Product Comparison
Compare reactions to regular dairy versus lactose-free versions. For example, eat a slice of regular cheddar cheese one day and a lactose-free alternative the next. Keep portions and timing consistent. If you tolerate the lactose-free option well but react to the regular version, this supports a lactose sensitivity diagnosis.
Do’s and Don’ts When Testing at Home
| Do’s | Don’ts |
|---|---|
| Keep a detailed symptom log including time, severity, and food intake | Assume all dairy-related discomfort is lactose intolerance |
| Use pure lactose sources (like milk) during challenge tests | Test while sick, stressed, or taking antibiotics |
| Gradually reintroduce dairy to assess tolerance thresholds | Consume large amounts of lactose if you’ve had severe reactions before |
| Read labels carefully to avoid hidden lactose | Ignore persistent symptoms after eliminating lactose—see a doctor |
Real-Life Example: Maria’s Experience
Maria, a 34-year-old teacher, experienced bloating and diarrhea after breakfast every day. She loved her morning latte and yogurt parfait but began suspecting dairy after reading about lactose intolerance. She eliminated all dairy for two weeks and felt dramatically better. To test, she drank a glass of milk on an empty stomach. Within 90 minutes, she developed cramping and gas—symptoms she hadn’t felt in weeks. Switching to lactose-free milk and plant-based yogurts allowed her to enjoy similar meals without discomfort. Her experience highlights how structured self-testing can reveal dietary triggers.
When to See a Doctor
Home tests are useful, but they aren't foolproof. Seek medical advice if:
- You experience weight loss, blood in stool, or fever—these suggest more serious conditions.
- Symptoms persist despite removing lactose.
- You're unsure whether it's lactose intolerance or a milk protein allergy (which can cause hives, wheezing, or swelling).
A healthcare provider may recommend a hydrogen breath test, which measures hydrogen levels in your breath after consuming lactose. Elevated levels indicate undigested lactose being fermented in the colon.
Frequently Asked Questions
Can you suddenly become lactose intolerant?
Yes. While many people inherit a predisposition, lactose intolerance can develop at any age. Illnesses like gastroenteritis, intestinal surgery, or conditions like celiac disease can temporarily or permanently reduce lactase production, leading to sudden onset symptoms.
Are there dairy products I can still eat if I'm lactose intolerant?
Absolutely. Many people tolerate hard cheeses (like cheddar or Swiss), butter, and fermented dairy (such as yogurt with live cultures) because they contain very little lactose. Lactose-free milk and enzyme supplements (like lactase pills) also allow safe consumption of dairy.
Is lactose intolerance the same as a milk allergy?
No. A milk allergy involves the immune system reacting to milk proteins (casein or whey) and can be life-threatening, especially in children. Lactose intolerance is a digestive issue and not dangerous, though uncomfortable. Allergies often cause hives, breathing problems, or anaphylaxis; intolerance causes gastrointestinal symptoms only.
Take Control of Your Digestive Health
Identifying lactose intolerance doesn’t require expensive tests or guesswork. By recognizing the key symptoms, using structured home trials, and understanding your body’s responses, you can gain clarity and control over your diet. Start with an elimination diet, document your results, and compare reactions to lactose-containing and lactose-free foods. Small changes can lead to significant improvements in comfort and daily well-being.









 浙公网安备
33010002000092号
浙公网安备
33010002000092号 浙B2-20120091-4
浙B2-20120091-4
Comments
No comments yet. Why don't you start the discussion?