Random muscle twitches—those sudden, involuntary contractions of a small part of a muscle or an entire muscle group—are more common than most people realize. You might feel them in your eyelid, calf, thumb, or even along your back. While often fleeting and harmless, persistent or worsening twitches can sometimes signal underlying health issues. Understanding the difference between benign fasciculations and those requiring medical attention is essential for peace of mind and timely care.
Understanding Muscle Twitches: The Science Behind Fasciculations
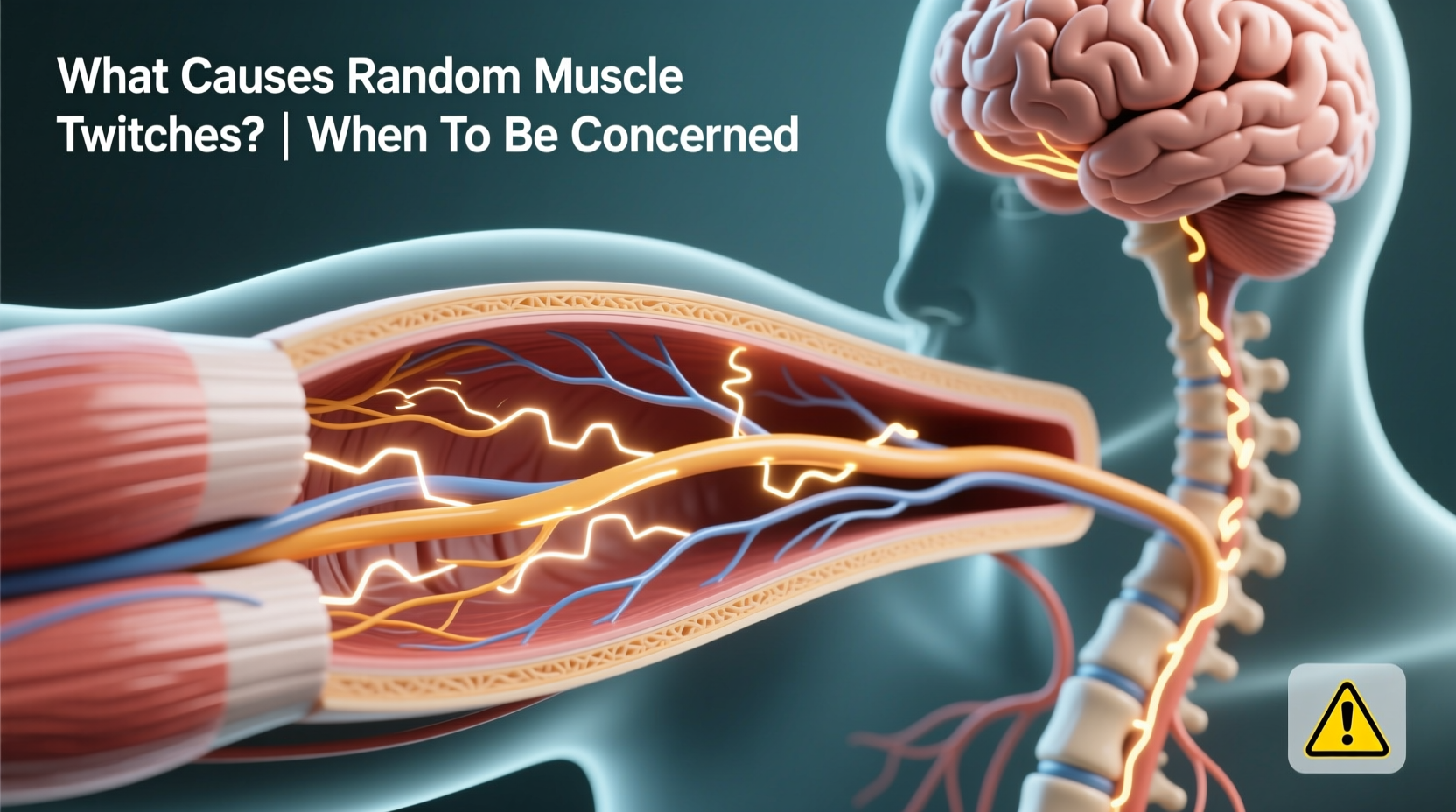
Muscle twitches, medically known as fasciculations, occur when a motor nerve fires spontaneously, causing a brief contraction in the muscle fibers it controls. These contractions are usually too weak to move a joint but strong enough to be felt under the skin. They differ from muscle cramps, which involve sustained contractions and often cause pain.
The nervous system constantly sends low-level signals to muscles to maintain tone and readiness. Occasionally, these signals misfire due to fatigue, stress, or chemical imbalances. In most cases, the twitch resolves on its own within seconds or minutes and doesn’t recur frequently.
“Most muscle twitches are benign and linked to lifestyle factors like stress, caffeine, or poor sleep. But if they persist beyond two weeks or spread across multiple muscle groups, it’s worth getting checked.” — Dr. Alan Reyes, Neurologist at Boston General Hospital
Common Causes of Random Muscle Twitches
The vast majority of muscle twitches are harmless and tied to everyday habits and conditions. Here are the most frequent triggers:
- Stress and anxiety: Elevated cortisol levels increase nerve excitability, making muscles more prone to spontaneous firing.
- Caffeine overconsumption: Found in coffee, energy drinks, and some medications, caffeine stimulates the central nervous system and can lead to jitteriness and twitching.
- Sleep deprivation: Chronic lack of rest disrupts normal neurological function, increasing twitch frequency, especially in the eyelids and limbs.
- Dehydration and electrolyte imbalance: Low levels of magnesium, calcium, potassium, or sodium impair nerve signaling and muscle control.
- Physical exertion: Intense workouts can cause micro-tears in muscle fibers and localized twitching during recovery.
- Nutritional deficiencies: Deficiencies in B vitamins (especially B12), vitamin D, or magnesium are commonly associated with neuromuscular irritability.
- Medication side effects: Certain drugs, including corticosteroids, diuretics, and asthma inhalers, may trigger twitching as a side effect.
When Should You Be Concerned? Red Flags to Watch For
While occasional twitches are normal, certain characteristics suggest a need for medical evaluation. Persistent or progressive symptoms could point to neurological conditions such as:
- Benign fasciculation syndrome (BFS)
- Peripheral neuropathy
- Multifocal motor neuropathy
- Amyotrophic lateral sclerosis (ALS)
- Multiple sclerosis (MS)
These disorders involve damage to motor neurons—the nerves that control voluntary muscles. Unlike everyday twitches, those linked to neurological disease typically follow a distinct pattern and are accompanied by other symptoms.
| Feature | Normal Twitch | Potentially Serious Twitch |
|---|---|---|
| Duration | Seconds to minutes; infrequent | Persistent (weeks to months), recurring daily |
| Location | Single spot (e.g., eyelid, calf) | Spreads to multiple areas (arm, leg, torso) |
| Associated Symptoms | None or mild fatigue | Muscle weakness, atrophy, cramping, numbness |
| Triggers | Caffeine, stress, exercise, lack of sleep | No clear trigger; occurs at rest |
| Response to Lifestyle Changes | Resolves with rest, hydration, reduced caffeine | Persists despite adjustments |
Key Warning Signs
If you experience any of the following, consult a neurologist:
- Twitching that lasts longer than two weeks without improvement
- Progressive muscle weakness (e.g., difficulty gripping objects or climbing stairs)
- Visible muscle shrinkage (atrophy)
- Fasciculations spreading from one body region to another
- Difficulty speaking, swallowing, or breathing
- Unexplained weight loss combined with twitching
Diagnosis and Medical Evaluation
If your symptoms raise concern, a healthcare provider will begin with a thorough history and physical exam. They’ll assess reflexes, muscle strength, coordination, and sensory function. Diagnostic tools may include:
- Blood tests: To check for electrolyte imbalances, thyroid dysfunction, vitamin deficiencies, or autoimmune markers.
- Electromyography (EMG): Measures electrical activity in muscles and helps distinguish between muscle and nerve disorders.
- Nerve conduction studies (NCS): Evaluates how well nerves transmit signals.
- MRI scans: Used if central nervous system involvement (like MS) is suspected.
It's important to note that EMG testing can detect abnormal activity even when symptoms seem minor. However, not all abnormal findings indicate serious disease—some people with BFS show EMG changes without progression.
Mini Case Study: Recognizing Early ALS Symptoms
Mark, a 52-year-old teacher, first noticed a twitch in his right thumb while grading papers. Over three months, the twitching spread to his forearm and shoulder. He also began dropping pens and struggling to open jars. Initially attributing it to overuse, he visited a neurologist after developing slurred speech. An EMG revealed widespread denervation, and further testing confirmed early-stage ALS. Prompt diagnosis allowed Mark to start treatment quickly, enroll in a clinical trial, and plan for future care needs.
This case highlights the importance of monitoring symptom progression. While most twitches aren’t ALS, the condition often begins subtly—with isolated fasciculations followed by weakness. Early intervention improves outcomes and access to supportive therapies.
Managing and Preventing Benign Muscle Twitches
For the majority of people, muscle twitches respond well to lifestyle modifications. Addressing root causes can reduce or eliminate episodes altogether.
Step-by-Step Guide to Reducing Twitch Frequency
- Reduce caffeine intake: Limit coffee, tea, and energy drinks to one serving per day or eliminate them temporarily to assess impact.
- Improve sleep hygiene: Aim for 7–9 hours nightly. Maintain a consistent bedtime, avoid screens before bed, and create a dark, cool sleeping environment.
- Stay hydrated: Drink water throughout the day, especially after exercise. Include electrolyte-rich foods like bananas, spinach, and avocados.
- Replenish key nutrients: Consider a blood test for magnesium, vitamin D, and B12. Supplementation may be advised if levels are low.
- Manage stress: Practice mindfulness, deep breathing, yoga, or meditation. Even 10 minutes daily can lower nervous system excitability.
- Stretch regularly: Gentle stretching after workouts or prolonged sitting helps relax tense muscles and prevent post-exercise twitching.
Checklist: Daily Habits to Minimize Twitching
- ✅ Drink at least 2 liters of water
- ✅ Consume magnesium-rich foods (nuts, seeds, leafy greens)
- ✅ Limit caffeine to morning hours only
- ✅ Get 7+ hours of quality sleep
- ✅ Perform 5–10 minutes of light stretching
- ✅ Practice stress-reducing techniques
- ✅ Avoid alcohol or consume in moderation
Frequently Asked Questions
Can dehydration really cause muscle twitches?
Yes. Dehydration affects the balance of electrolytes like sodium, potassium, and magnesium, all of which are critical for proper nerve signaling and muscle contraction. Even mild dehydration can increase twitch frequency, particularly after exercise or in hot weather.
Are eye twitches different from other muscle twitches?
Eyelid twitching (myokymia) is very common and usually caused by stress, fatigue, or excessive screen time. It tends to resolve on its own within days. However, persistent eyelid spasms involving the entire orbicularis oculi muscle (blepharospasm) may require medical evaluation, especially if they interfere with vision.
Is there a link between anxiety and muscle twitching?
Definitely. Anxiety increases sympathetic nervous system activity, leading to heightened muscle tension and nerve sensitivity. People with generalized anxiety or panic disorders often report widespread twitching, especially during high-stress periods. Managing anxiety through therapy, medication, or relaxation techniques often reduces twitching significantly.
Conclusion: Listen to Your Body, Act When Needed
Random muscle twitches are rarely dangerous, but they shouldn't be ignored when patterns change or new symptoms appear. Most cases stem from manageable lifestyle factors—stress, poor sleep, or nutrient gaps—that respond well to simple interventions. Paying attention to your body’s signals allows you to act early, whether that means adjusting your habits or seeking expert advice.
If twitching persists beyond a few weeks, spreads across muscle groups, or comes with weakness or atrophy, don’t wait. A neurologist can help determine whether the cause is benign or requires further investigation. Knowledge and awareness are powerful tools—use them to protect your long-term health.









 浙公网安备
33010002000092号
浙公网安备
33010002000092号 浙B2-20120091-4
浙B2-20120091-4
Comments
No comments yet. Why don't you start the discussion?