If you find yourself catching colds every few weeks, battling fatigue, or struggling with recurring infections, you’re not alone. Many people ask, “Why am I always sick?” While occasional illness is normal—especially during flu season—frequent sickness may signal an underlying issue. Understanding the root causes can help you take control of your health and know when it’s time to consult a medical professional.
Common Causes of Frequent Illness
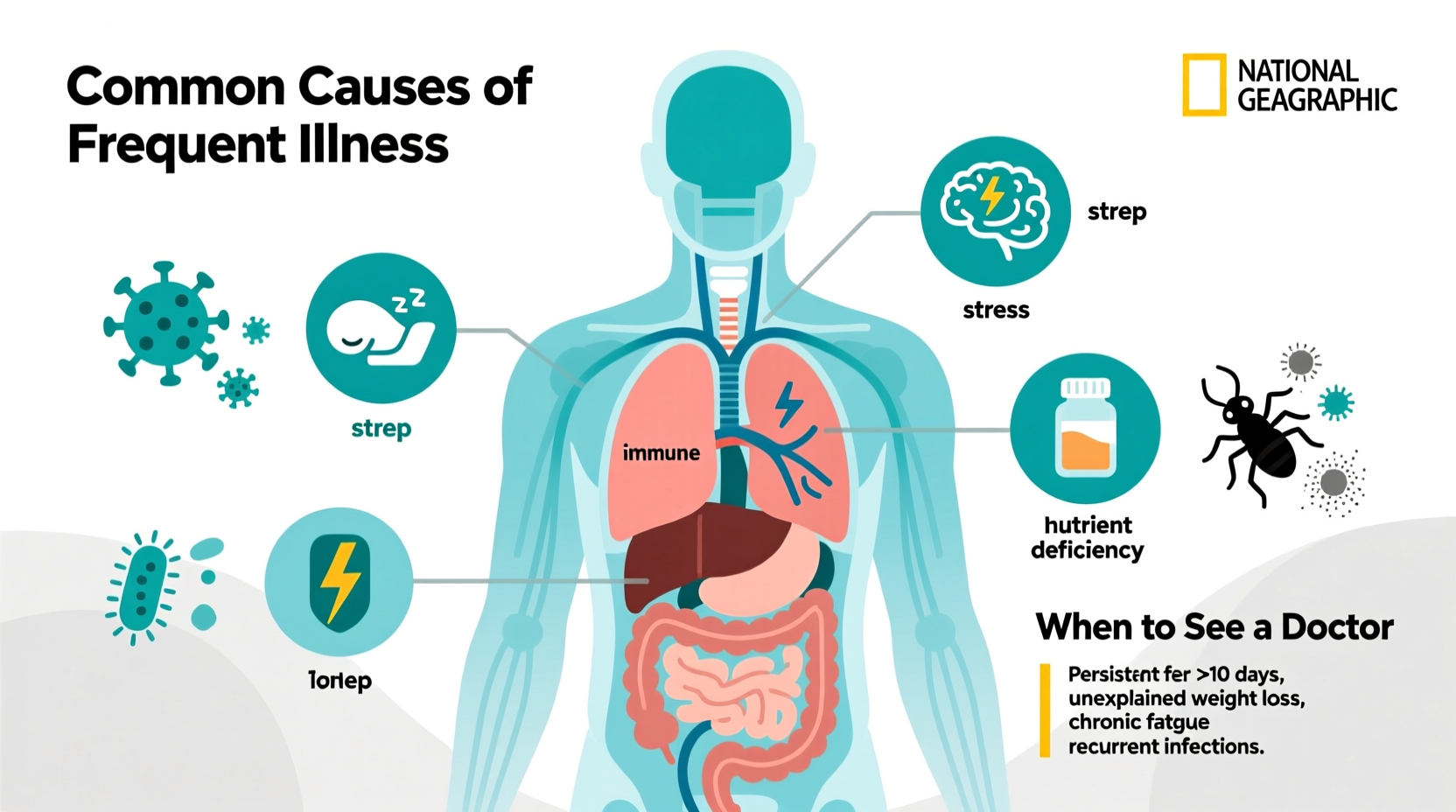
Frequent illness isn’t just bad luck. It often reflects lifestyle habits, environmental exposures, or physiological imbalances that weaken your immune system over time. Here are some of the most prevalent reasons people stay sick more than they should:
- Poor Sleep Habits: Chronic sleep deprivation disrupts immune function. Adults who consistently get less than 7 hours of sleep per night are three times more likely to catch a cold.
- Nutritional Deficiencies: Low levels of vitamin D, zinc, iron, and vitamin C impair immune responses. Diets high in processed foods and sugar also promote inflammation.
- Chronic Stress: Prolonged stress elevates cortisol, which suppresses white blood cell activity and increases susceptibility to infections.
- Lack of Physical Activity: Sedentary lifestyles reduce circulation of immune cells. Moderate exercise, however, boosts immune surveillance.
- Exposure to Germs: Working in healthcare, schools, or public-facing roles increases contact with pathogens.
- Underlying Medical Conditions: Autoimmune disorders, diabetes, thyroid issues, and chronic lung diseases can compromise immunity.
- Medications: Long-term use of corticosteroids, chemotherapy drugs, or immunosuppressants weakens the body's defense mechanisms.
When Lifestyle Isn't Enough: Hidden Health Issues
Sometimes, even with healthy habits, you may still feel unwell. Certain conditions mimic or directly cause frequent illness and are often overlooked:
- Vitamin D Deficiency: Affects up to 40% of adults in the U.S. Linked to increased respiratory infections.
- Food Sensitivities: Chronic low-grade inflammation from gluten, dairy, or other allergens can exhaust immune resources.
- Gut Health Imbalance: 70% of your immune system resides in the gut. Dysbiosis (microbial imbalance) impairs pathogen defense.
- Chronic Fatigue Syndrome (ME/CFS): Characterized by extreme fatigue and post-exertional malaise, often mistaken for repeated viral infections.
- Primary Immunodeficiency Disorders: Rare but serious conditions like Common Variable Immunodeficiency (CVID) where the body fails to produce adequate antibodies.
“Recurrent infections shouldn’t be dismissed as ‘just a weak immune system.’ We’ve diagnosed patients in their 30s with lifelong undiagnosed immunodeficiencies because symptoms were normalized.” — Dr. Lena Torres, Immunologist at Boston General Hospital
Red Flags: When to See a Doctor
Not every cold warrants a doctor visit, but certain patterns suggest it’s time to seek medical evaluation. Keep track of frequency, severity, and recovery time. The following signs indicate you should schedule an appointment:
| Symptom Pattern | Normal | Concerning – See a Doctor |
|---|---|---|
| Colds per year | 2–4 (adults) | 6+ with prolonged duration (>10 days) |
| Antibiotics needed | Rarely | 4+ times per year |
| Fever duration | 1–3 days | Recurrent fevers lasting >5 days without clear cause |
| Recovery time | Gradual improvement in 7–10 days | Worsening after initial improvement |
| Other symptoms | Occasional sore throat or congestion | Unexplained weight loss, night sweats, swollen lymph nodes |
Diagnostic Steps Your Doctor May Take
If you meet any of the concerning criteria above, your physician might recommend:
- Blood tests (CBC, CRP, ESR) to check for infection or inflammation
- Immune panel testing (immunoglobulin levels, vaccine response)
- Vitamin and mineral screening (especially D, B12, zinc, iron)
- Allergy testing if sinus or respiratory symptoms dominate
- Referral to an immunologist or infectious disease specialist
Real-Life Example: Sarah’s Story
Sarah, a 34-year-old teacher, came down with bronchitis four times in one winter. She assumed it was due to being around kids. But after missing two weeks of work and failing to improve with antibiotics, she consulted an internal medicine specialist. Blood work revealed low IgG levels and undiagnosed celiac disease. Once she started a gluten-free diet and received immunoglobulin support, her infection rate dropped dramatically. Her case highlights how underlying conditions can masquerade as “being prone to colds.”
Action Plan: What You Can Do Now
Before jumping to worst-case scenarios, take proactive steps to support your immune system. Use this checklist to assess and improve your daily habits:
- ✅ Aim for 7–9 hours of uninterrupted sleep nightly
- ✅ Eat at least 5 servings of colorful fruits and vegetables daily
- ✅ Drink plenty of water—dehydration slows mucosal defenses
- ✅ Exercise moderately for 30 minutes, 4–5 times per week
- ✅ Manage stress with mindfulness, yoga, or breathing exercises
- ✅ Wash hands frequently, especially during cold and flu season
- ✅ Get annual flu shots and stay up-to-date on other vaccines
- ✅ Limit alcohol and avoid smoking or vaping
Frequently Asked Questions
Can anxiety make me physically sick more often?
Yes. Chronic anxiety triggers sustained release of stress hormones like cortisol and adrenaline, which over time suppress immune cell production and function. This makes you more vulnerable to viruses and slows healing.
Is it normal to get sick after traveling?
Moderately. Airports and planes expose you to concentrated germs, dry air, and circadian disruption. However, getting sick after *every* trip isn’t normal. Consider boosting immunity before travel with extra sleep, hydration, and possibly zinc or vitamin C supplementation.
Do frequent cold sores mean my immune system is weak?
Recurrent herpes simplex virus (HSV-1) outbreaks can be triggered by stress, sun exposure, or illness. While occasional flare-ups are common, frequent episodes (more than 6 per year) may indicate immune strain or deficiency.
Conclusion: Listen to Your Body
Feeling sick all the time isn’t something you should accept as normal. While lifestyle factors play a major role, persistent illness can be a signal from your body that something deeper needs attention. By improving sleep, nutrition, and stress management—and knowing when to seek medical advice—you empower yourself to break the cycle of constant infection.









 浙公网安备
33010002000092号
浙公网安备
33010002000092号 浙B2-20120091-4
浙B2-20120091-4
Comments
No comments yet. Why don't you start the discussion?