Feeling nauseous or on the verge of vomiting after eating is more than just an occasional discomfort—it can disrupt daily life, affect nutrition, and signal underlying health issues. While it’s normal to feel slightly full after a large meal, persistent nausea following food intake is not something to ignore. This article explores the most common reasons behind post-meal vomiting sensations, backed by medical insights, and provides practical, science-based solutions to help you regain control over your digestive health.
Common Causes of Nausea After Eating
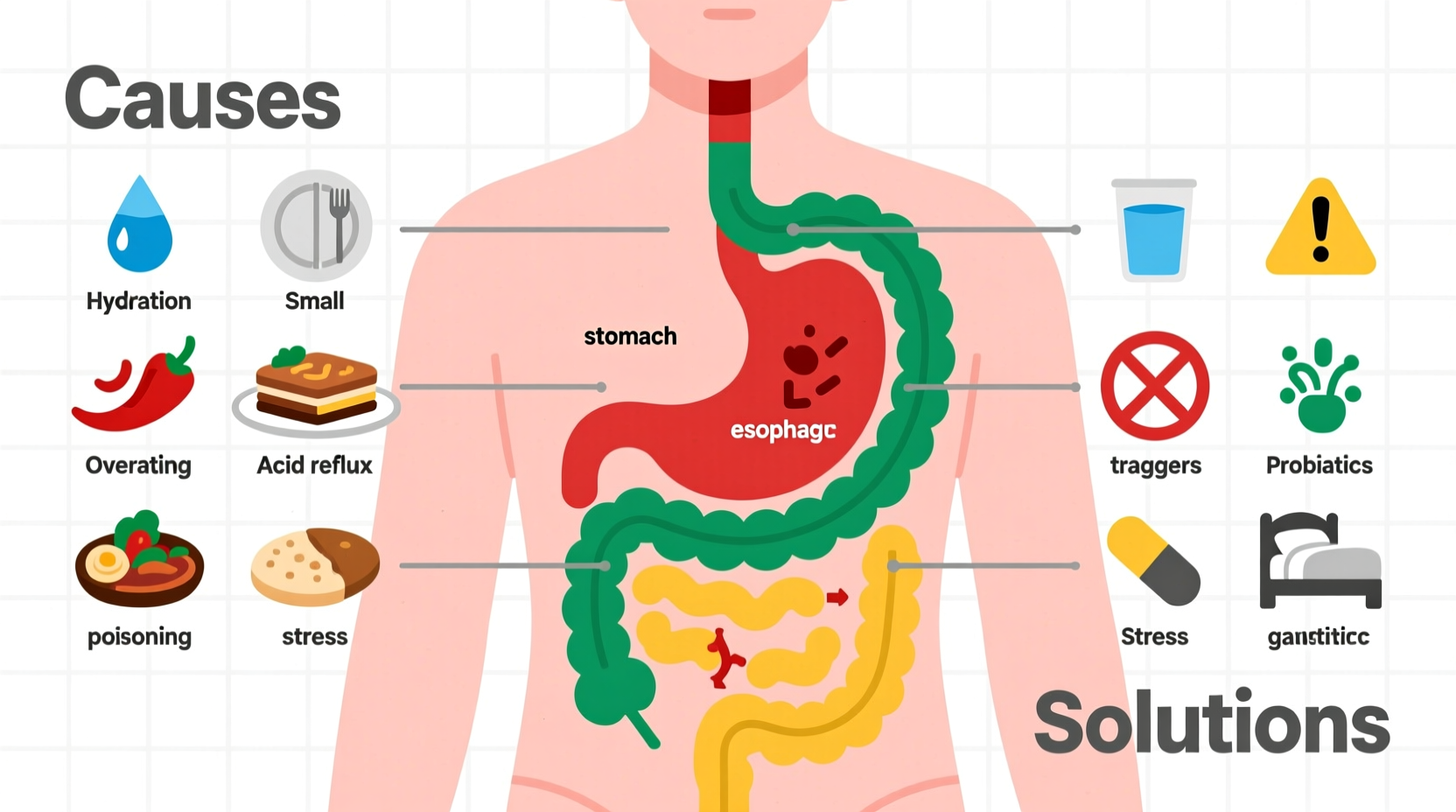
Nausea that arises shortly after eating can stem from a range of factors—some related to diet and eating habits, others tied to chronic medical conditions. Understanding the root cause is essential for effective treatment.
- Overeating: Consuming large portions stretches the stomach, triggering pressure and discomfort that can lead to nausea.
- Gastroesophageal Reflux Disease (GERD): Stomach acid flows back into the esophagus, causing irritation, heartburn, and a sensation of needing to vomit.
- Gastroparesis: A condition where the stomach empties too slowly due to nerve damage, often seen in people with diabetes.
- Food Intolerances: Lactose intolerance, gluten sensitivity, or reactions to certain food additives can cause bloating, gas, and nausea.
- Pregnancy: Hormonal changes, especially in the first trimester, frequently cause morning sickness and post-meal nausea.
- Anxiety and Stress: The gut-brain connection means emotional stress can directly impact digestion and trigger nausea.
- Gallbladder Disorders: Gallstones or inflammation impair bile release, making fat digestion difficult and leading to nausea after fatty meals.
- Peptic Ulcers: Sores in the stomach lining or duodenum can become irritated by food, especially acidic or spicy items.
When to Seek Medical Attention
While occasional nausea may resolve on its own, certain symptoms indicate the need for prompt medical evaluation. Ignoring these signs could delay diagnosis of serious conditions.
“Recurrent nausea after meals shouldn’t be dismissed as ‘just indigestion.’ It can be a red flag for gastrointestinal disorders, metabolic imbalances, or even cardiac issues.” — Dr. Lena Patel, Gastroenterologist
Seek immediate medical advice if you experience any of the following:
- Vomiting blood or material that looks like coffee grounds
- Severe abdominal pain or cramping
- Unintentional weight loss
- Frequent episodes lasting more than a few days
- Symptoms that worsen over time
- Dizziness, rapid heartbeat, or fainting alongside nausea
Effective Solutions and Management Strategies
Treating post-meal nausea starts with identifying triggers and modifying lifestyle and dietary habits. In many cases, simple adjustments yield significant relief.
1. Adjust Your Eating Habits
How you eat is just as important as what you eat. Slowing down and being mindful during meals supports better digestion.
- Eat smaller, more frequent meals instead of three large ones.
- Chew food thoroughly to reduce the digestive burden.
- Avoid lying down within 2–3 hours after eating to prevent reflux.
- Drink fluids between meals, not during, to avoid stomach distension.
2. Modify Your Diet
Certain foods are more likely to trigger nausea. Tailoring your diet can provide quick relief.
| Foods to Limit or Avoid | Better Alternatives |
|---|---|
| Fried, greasy, or high-fat foods | Grilled, steamed, or baked lean proteins |
| Spicy dishes | Mild seasonings like ginger, turmeric, or fennel |
| Citrus fruits, tomatoes, vinegar | Low-acid fruits like bananas, melons |
| Caffeine and carbonated drinks | Herbal teas (peppermint, chamomile), water |
| Dairy (if lactose intolerant) | Lactose-free milk or plant-based alternatives |
3. Address Underlying Conditions
If nausea persists despite dietary changes, treating the root medical issue is crucial. Common interventions include:
- Medications: Proton pump inhibitors (PPIs) for GERD, prokinetics for gastroparesis, or antihistamines for vestibular-related nausea.
- Blood Tests: To check for infections, liver function, pancreatic enzymes, or electrolyte imbalances.
- Imaging: Ultrasound for gallbladder issues, endoscopy for ulcers or inflammation.
Mini Case Study: Managing Chronic Post-Meal Nausea
Sarah, a 34-year-old office worker, began experiencing nausea about 20 minutes after every lunch. She initially assumed it was stress-related, but the problem persisted for weeks. After tracking her meals, she noticed symptoms only occurred after eating fried chicken sandwiches and soda.
She consulted her doctor, who ordered an ultrasound and diagnosed mild gallstones. Sarah was advised to adopt a low-fat diet and avoid greasy foods. Within two weeks of switching to grilled fish, vegetables, and herbal tea, her symptoms disappeared. This case highlights how specific food triggers—especially fats—can exacerbate underlying conditions and how targeted dietary changes can bring fast relief.
Step-by-Step Guide to Reducing Post-Meal Nausea
Follow this structured approach to identify and eliminate the causes of your nausea:
- Week 1: Track Symptoms – Record everything you eat, portion sizes, timing, and any nausea episodes. Note intensity and duration.
- Week 2: Eliminate Common Triggers – Remove fried foods, caffeine, carbonation, and heavy spices. Eat bland, easily digestible meals.
- Week 3: Reintroduce Foods Gradually – Add one potential trigger back at a time to test tolerance.
- Week 4: Consult a Professional – If symptoms persist, schedule an appointment with a gastroenterologist or registered dietitian.
- Ongoing: Maintain Healthy Habits – Stick to small meals, stay hydrated, manage stress, and avoid late-night eating.
FAQ
Can anxiety really cause nausea after eating?
Yes. Anxiety activates the sympathetic nervous system, which can slow digestion and increase stomach acid production. This imbalance often leads to nausea, bloating, or a “knot” in the stomach, especially during or after meals.
Is it normal to feel nauseous after breakfast?
Occasional mild nausea may happen due to dehydration or eating too quickly. However, consistent morning nausea could point to low blood sugar, acid reflux, or pregnancy. Persistent symptoms warrant evaluation.
What over-the-counter remedies help with post-meal nausea?
Antacids (like Tums or Maalox) can relieve acid-related nausea. Bismuth subsalicylate (Pepto-Bismol) helps with upset stomach and mild gastritis. Always follow label instructions and consult a doctor if using long-term.
Checklist: What You Can Do Today
- ✅ Eat slower and chew each bite thoroughly
- ✅ Reduce portion sizes by using a smaller plate
- ✅ Avoid reclining immediately after meals
- ✅ Replace coffee with ginger or chamomile tea
- ✅ Drink a glass of water 30 minutes before eating
- ✅ Write down everything you eat and any symptoms
- ✅ Schedule a doctor’s visit if nausea lasts beyond a week
Conclusion
Feeling like vomiting after eating is not something you should simply endure. Whether it's caused by poor eating habits, food sensitivities, or a medical condition, there are proven ways to find relief. By paying attention to your body’s signals, adjusting your diet, and seeking professional guidance when needed, you can restore comfort and confidence around mealtimes. Don’t let nausea dictate your relationship with food—take action today to understand and resolve the cause.









 浙公网安备
33010002000092号
浙公网安备
33010002000092号 浙B2-20120091-4
浙B2-20120091-4
Comments
No comments yet. Why don't you start the discussion?