Swollen feet after prolonged standing are common, especially among people who work on their feet—nurses, retail workers, teachers, and construction laborers. While mild swelling may seem like a minor inconvenience, persistent or severe edema can signal underlying health issues. Understanding the causes, recognizing warning signs, and knowing when to consult a healthcare provider are essential steps in maintaining long-term circulatory and musculoskeletal health.
How Prolonged Standing Leads to Foot Swelling
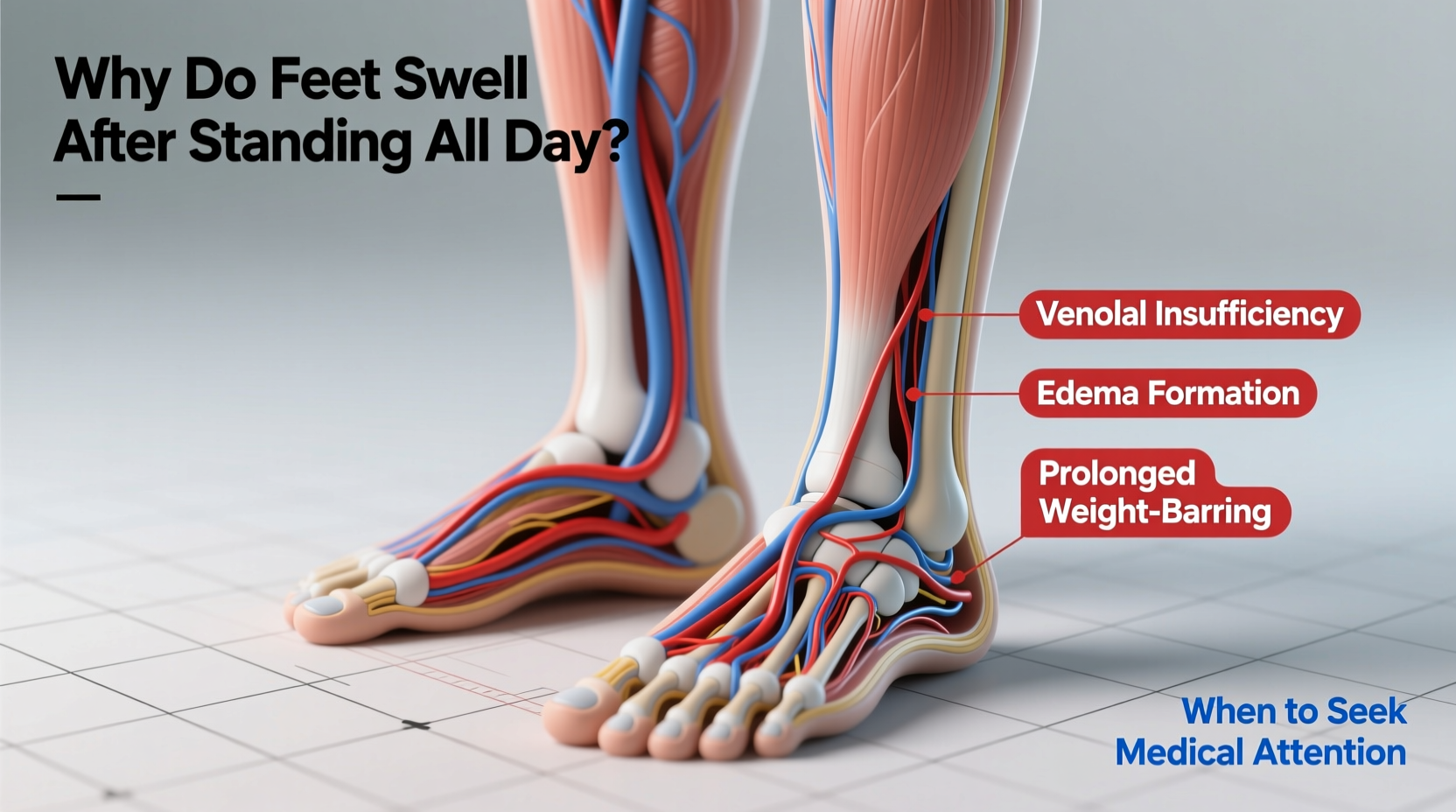
When you stand for extended periods, gravity pulls blood and fluid into the lower extremities. The veins in your legs must work harder to return blood to the heart, and if the venous valves or calf muscle pump aren't functioning efficiently, fluid begins to accumulate in the tissues of the feet and ankles—a condition known as dependent edema.
The lymphatic system also plays a role. It helps drain excess interstitial fluid, but prolonged immobility reduces its effectiveness. As fluid pools in the feet, tissues expand, causing tightness, puffiness, and discomfort. This type of swelling typically improves with elevation and rest but can become chronic without intervention.
The Role of Circulation and Venous Insufficiency
Chronic venous insufficiency (CVI) is a major contributor to foot swelling in people who stand for long hours. In CVI, damaged or weakened vein valves fail to prevent blood from flowing backward, leading to pooling in the lower legs. Over time, this increases pressure in the veins, damages capillaries, and allows fluid to leak into surrounding tissues.
Symptoms include:
- Swelling that worsens throughout the day
- Achy, heavy legs
- Visible varicose veins
- Itching or skin discoloration around the ankles
- Night cramps
“Prolonged standing without movement significantly increases hydrostatic pressure in leg veins. Over years, this can lead to permanent venous damage.” — Dr. Alan Reyes, Vascular Medicine Specialist
Common Causes of Post-Standing Foot Swelling
While gravity and poor circulation are primary culprits, several other factors contribute to or exacerbate foot swelling after standing:
- Heat exposure: Warm temperatures cause blood vessels to dilate, increasing fluid leakage into tissues.
- High-sodium diet: Excess salt leads to water retention, worsening edema.
- Pregnancy: Hormonal changes and increased blood volume raise susceptibility to swelling, especially in the third trimester.
- Obesity: Extra body weight increases pressure on leg veins and reduces mobility, impairing circulation.
- Medications: Certain drugs—including calcium channel blockers, NSAIDs, and some antidepressants—can cause fluid retention.
- Lack of compression support: Not wearing supportive footwear or compression socks reduces venous return efficiency.
When Swelling Is More Than Just Tired Feet
Not all foot swelling is benign. Some cases point to systemic conditions requiring medical evaluation. Persistent or asymmetric swelling should never be ignored. Below are red flags indicating the need for prompt assessment.
| Symptom | May Indicate | Action Required |
|---|---|---|
| Swelling only in one leg | DVT (deep vein thrombosis) | Seek emergency care |
| Pain, warmth, redness in swollen area | Infection or clot | Immediate evaluation |
| Shortness of breath with swelling | Heart failure | Emergency |
| Swelling with abdominal bloating | Liver or kidney disease | See doctor within 48 hours |
| No improvement after rest and elevation | Chronic venous disease or lymphedema | Consult vascular specialist |
Real-Life Example: Maria’s Experience
Maria, a 47-year-old schoolteacher, noticed her feet swelling daily after eight-hour shifts. Initially, she dismissed it as normal fatigue. She wore flat shoes and rarely sat during class. Over six months, the swelling became more pronounced, and her ankles developed darkened, leathery skin—a condition called stasis dermatitis.
After experiencing leg pain and difficulty removing her shoes, she consulted a vascular specialist. An ultrasound revealed moderate chronic venous insufficiency. With prescription compression stockings, lifestyle adjustments, and regular walking breaks, Maria reduced her symptoms by 70% within two months.
Her case illustrates how seemingly minor daily discomfort can progress into chronic vascular issues without early intervention.
Preventive Strategies and Daily Management Tips
You don’t have to resign yourself to swollen feet if your job requires standing. Several practical measures can reduce fluid accumulation and improve circulation.
Step-by-Step Guide to Reduce Swelling During Long Shifts
- Wear compression socks (15–20 mmHg): Put them on before getting out of bed to maximize effectiveness.
- Choose supportive footwear: Shoes with arch support, cushioning, and a slight heel reduce strain on veins.
- Take micro-breaks: Every hour, walk for 2–3 minutes or perform seated calf raises.
- Stay hydrated: Drinking enough water helps regulate sodium balance and reduces fluid retention.
- Limit salt intake: Avoid processed foods high in sodium, especially before long shifts.
- Elevate legs post-shift: Lie down with legs raised above heart level for 15–20 minutes.
- Cool down: Use cold foot soaks (not ice-cold) to constrict blood vessels and reduce inflammation.
Do’s and Don’ts for Managing Foot Swelling
| Do | Don't |
|---|---|
| Move regularly—even small steps help | Sit or stand completely still for hours |
| Wear graduated compression stockings | Use tight elastic bands or non-medical “shaping” socks |
| Drink herbal teas like dandelion (natural diuretic) | Overuse over-the-counter diuretics without medical advice |
| Monitor changes in shoe tightness or skin texture | Ignore persistent indentations from sock lines |
| Track symptoms in a journal | Assume all swelling is normal |
When to See a Doctor: Warning Signs You Shouldn’t Ignore
Occasional swelling that resolves overnight is usually harmless. However, certain patterns indicate underlying pathology. Seek medical attention if you experience any of the following:
- Swelling lasts more than 24 hours despite rest and elevation.
- One leg is significantly more swollen than the other—this could indicate a deep vein thrombosis (DVT), a potentially life-threatening clot.
- Chest pain or shortness of breath accompanying swelling—this may suggest heart failure or pulmonary embolism.
- Changes in skin color or texture, such as redness, shininess, or ulceration near the ankle.
- Pitting edema that leaves an indentation when pressed and doesn’t rebound quickly.
- Swelling accompanied by fatigue, confusion, or decreased urination, which may point to kidney dysfunction.
Your primary care physician may refer you to a cardiologist, nephrologist, or vascular specialist depending on suspected causes. Diagnostic tools may include:
- Blood tests (to check kidney, liver, and heart function)
- Urinalysis (for proteinuria indicating kidney issues)
- Doppler ultrasound (to assess blood flow and rule out clots)
- Echocardiogram (if heart failure is suspected)
Frequently Asked Questions
Is foot swelling after standing always dangerous?
No, mild swelling after prolonged standing is common and often resolves with rest, elevation, and movement. However, if it becomes frequent, painful, or asymmetrical, it warrants medical evaluation to rule out serious conditions like DVT or heart disease.
Can drinking more water reduce swelling?
Yes. Dehydration triggers the body to retain sodium and fluid, worsening edema. Staying well-hydrated supports kidney function and helps flush excess sodium, reducing water retention.
Are compression socks safe for daily use?
Yes, properly fitted graduated compression socks (15–20 mmHg) are safe and recommended for people who stand or sit for long periods. However, individuals with peripheral artery disease or severe neuropathy should consult a doctor before use.
Checklist: What to Do If Your Feet Swell After Standing
- ✅ Evaluate the frequency and duration of swelling.
- ✅ Note any associated symptoms (pain, warmth, shortness of breath).
- ✅ Try elevation, hydration, and gentle movement for relief.
- ✅ Wear supportive shoes and consider compression socks.
- ✅ Monitor for pitting edema or skin changes.
- ✅ Schedule a doctor’s visit if swelling persists beyond 24 hours or affects only one leg.
- ✅ Keep a symptom log to share with your healthcare provider.
Conclusion: Listen to Your Body Before Problems Escalate
Foot swelling after standing is not something you should simply endure. While often benign, it can be an early signal of circulatory, cardiac, or renal issues. By adopting preventive habits—like wearing compression gear, staying active, and managing diet—you can protect your vascular health. More importantly, recognizing when swelling crosses the line from normal to concerning can make a critical difference in preventing complications.









 浙公网安备
33010002000092号
浙公网安备
33010002000092号 浙B2-20120091-4
浙B2-20120091-4
Comments
No comments yet. Why don't you start the discussion?