Many people experience a sudden flush in their face after drinking alcohol—skin turns pink or red, often accompanied by warmth or discomfort. While it may seem harmless, facial redness after drinking can signal deeper physiological reactions, particularly related to how the body processes alcohol. This response, commonly known as \"alcohol flush,\" affects millions worldwide, especially those of East Asian descent. Understanding the root causes and learning how to manage or prevent this reaction is essential for both comfort and long-term health.
The Science Behind Alcohol-Induced Facial Redness
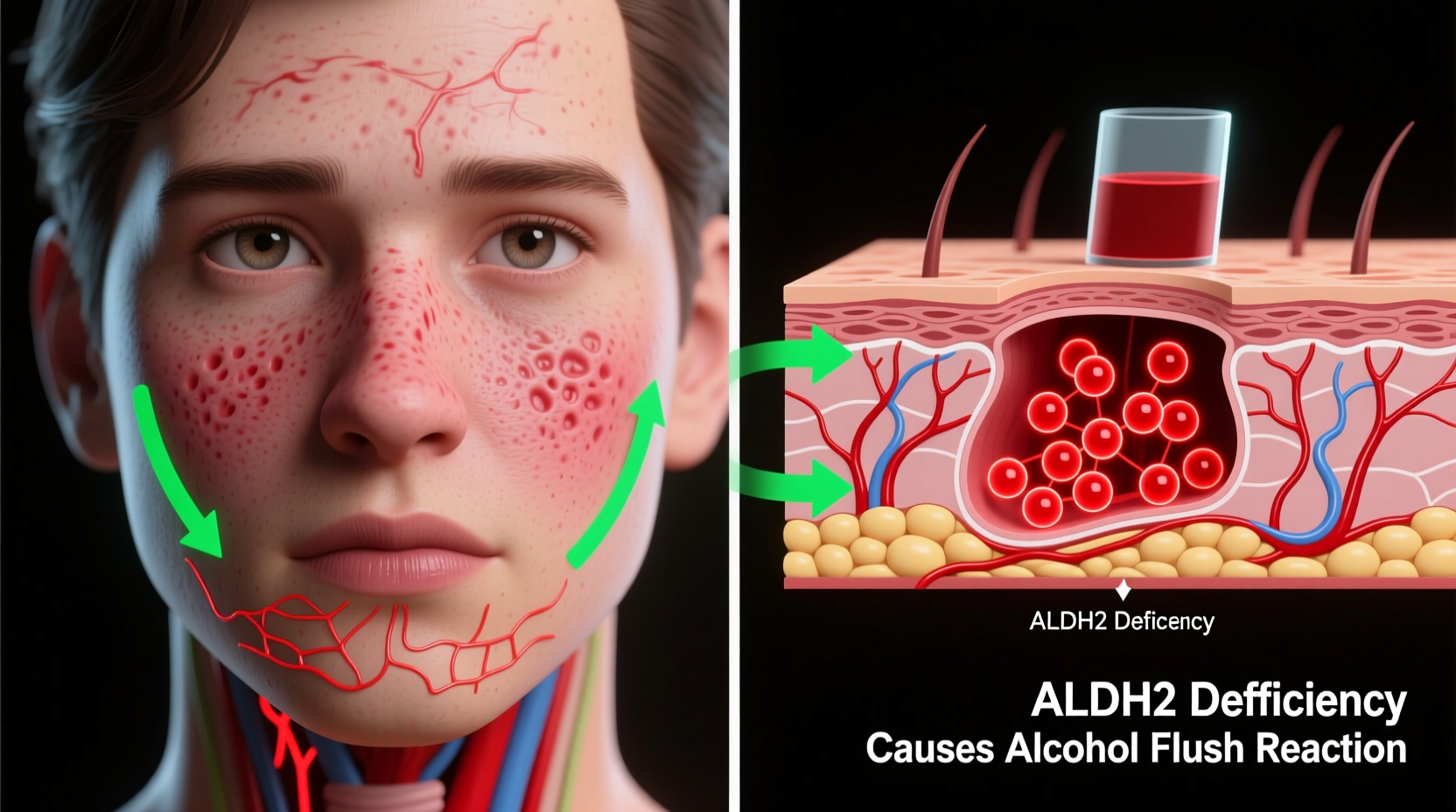
Facial flushing after drinking is primarily caused by the buildup of acetaldehyde, a toxic byproduct of alcohol metabolism. When you consume alcohol, your liver breaks it down in two key steps:
- Alcohol (ethanol) is converted into acetaldehyde by an enzyme called alcohol dehydrogenase (ADH).
- Acetaldehyde is then broken down into acetate by aldehyde dehydrogenase 2 (ALDH2), which the body uses or excretes.
The problem arises when ALDH2 is deficient or less active. In individuals with a genetic variation—most commonly found in people of Chinese, Japanese, or Korean heritage—the ALDH2 enzyme works inefficiently or not at all. As a result, acetaldehyde accumulates rapidly in the bloodstream, causing blood vessels in the face to dilate, leading to redness, warmth, and sometimes itching or rapid heartbeat.
“Acetaldehyde is a recognized carcinogen. When it builds up due to poor metabolism, it doesn’t just cause redness—it increases cancer risk over time.” — Dr. Sarah Kim, Molecular Toxicologist, National Institute on Alcohol Abuse and Health
Who Is Most at Risk?
While anyone can experience mild flushing from alcohol, certain populations are genetically predisposed. The ALDH2 deficiency affects approximately 35–40% of East Asians. However, cases have also been reported in other ethnic groups, though less frequently.
Symptoms typically appear within minutes of consuming alcohol and include:
- Redness in the face, neck, or shoulders
- Warmth or burning sensation on the skin
- Nasal congestion
- Rapid heartbeat (tachycardia)
- Nausea or headache
Health Risks Associated with Chronic Flushing
Repeated episodes of alcohol-induced flushing aren't just uncomfortable—they can be dangerous. Long-term exposure to high acetaldehyde levels increases the risk of several serious conditions:
- Esophageal Cancer: Studies show that individuals with ALDH2 deficiency who drink regularly have a significantly higher risk of developing esophageal cancer—up to 6–10 times greater than non-flushers.
- Hypertension: Vasodilation from acetaldehyde can strain the cardiovascular system, especially when combined with frequent alcohol use.
- Liver Stress: Even moderate drinking can overwhelm a compromised metabolic pathway, increasing oxidative stress on the liver.
Despite these risks, many dismiss the flush as a benign reaction. Medical professionals warn against normalizing this symptom, especially if drinking continues despite discomfort.
Effective Prevention and Management Strategies
There is no cure for ALDH2 deficiency, but several strategies can help minimize symptoms and protect long-term health.
Step-by-Step Guide to Reduce or Prevent Flushing
- Limit or Eliminate Alcohol Consumption: The most effective way to prevent flushing is to avoid alcohol altogether. For those with severe deficiency, even small amounts trigger strong reactions.
- Choose Low-Alcohol or Non-Alcoholic Beverages: Opt for drinks with minimal ethanol content. Non-alcoholic beer or wine may still contain trace alcohol, so read labels carefully.
- Eat Before Drinking: Consuming food slows alcohol absorption, giving your body more time to process it—even if inefficiently.
- Stay Hydrated: Drink water between alcoholic beverages to support detoxification and reduce acetaldehyde concentration.
- Avoid Triggers Like Histamine-Rich Drinks: Red wine, champagne, and aged spirits contain histamines and congeners that worsen flushing in sensitive individuals.
| Do’s | Don’ts |
|---|---|
| Drink water alongside any alcohol | Use antihistamines to mask flushing (they don’t stop acetaldehyde buildup) |
| Eat protein-rich foods before drinking | Engage in binge drinking to “get used” to the flush |
| Opt for clear spirits like vodka (lower congener content) | Ignore persistent symptoms like nausea or chest pain |
| Track your reactions in a journal | Assume all redness is harmless |
Real-Life Example: A Case Study
Jin, a 29-year-old software engineer of Korean descent, had always turned bright red after just one beer. He assumed it was normal until a routine checkup revealed elevated liver enzymes. His doctor asked about his drinking habits. Although he only drank socially, the cumulative effect of weekly gatherings was taking a toll.
After genetic testing confirmed ALDH2 deficiency, Jin decided to cut out alcohol entirely. Within three months, his liver markers normalized, and he reported better sleep and energy levels. “I thought I was just ‘bad at drinking,’” he said. “Now I realize my body was warning me all along.”
Common Myths and Misconceptions
Several myths persist about alcohol flushing, often leading people to make risky choices:
- Myth: “Building tolerance reduces flushing.”
Truth: Tolerance doesn’t fix the enzyme deficiency. Continued drinking increases cancer risk. - Myth: “Taking antihistamines prevents harm.”
Truth: Some people take H2 blockers like famotidine to reduce redness, but this masks symptoms without reducing acetaldehyde toxicity. - Myth: “Only heavy drinkers need to worry.”
Truth: Even light drinking is harmful for those with ALDH2 deficiency due to impaired metabolism.
Frequently Asked Questions
Can you suddenly develop alcohol flush later in life?
True ALDH2 deficiency is genetic and present from birth, but some people notice flushing more prominently as they age due to changes in liver function, medications, or hormonal shifts. Sudden onset of redness could also indicate rosacea or an allergic reaction, so consult a doctor if symptoms change.
Is facial redness the same as an alcohol allergy?
No. An alcohol allergy involves the immune system and can cause hives, swelling, or difficulty breathing. Flushing is a metabolic issue, not an immune response. However, both require medical attention if severe.
Are there supplements that help break down acetaldehyde?
Some products claim to boost ALDH2 activity or provide antioxidants like vitamin B complex or N-acetylcysteine (NAC). While NAC supports liver detox pathways, no supplement can fully compensate for genetic deficiency. Relying on them to drink safely is not recommended by health experts.
Final Checklist: Managing Alcohol Flush Responsibly
- ✔ Recognize facial redness as a potential sign of ALDH2 deficiency
- ✔ Avoid using medications to mask symptoms
- ✔ Limit alcohol intake or abstain completely if flushing occurs
- ✔ Choose lower-congener drinks if consuming occasionally
- ✔ Consult a healthcare provider for genetic testing or liver evaluation
- ✔ Educate friends and family about your sensitivity to reduce social pressure
Conclusion: Listen to Your Body
Your face turning red after drinking isn't just an aesthetic quirk—it's a biological red flag. The body uses flushing as a warning system, signaling that toxins are accumulating faster than they can be removed. Ignoring this signal can lead to serious long-term consequences, including increased cancer risk and organ damage.
Whether you choose to modify your drinking habits or eliminate alcohol altogether, the most important step is awareness. Make informed decisions based on your body’s responses, not social expectations. Your health is far more valuable than fitting in at a party.









 浙公网安备
33010002000092号
浙公网安备
33010002000092号 浙B2-20120091-4
浙B2-20120091-4
Comments
No comments yet. Why don't you start the discussion?