A burning sensation in the nose can be more than just a minor irritation—it can signal underlying inflammation, infection, or environmental triggers affecting the delicate mucous membranes inside your nasal passages. This discomfort often extends into the sinuses, creating a persistent, stinging feeling that worsens with breathing, weather changes, or allergen exposure. While occasional nasal burning is common, recurring or severe symptoms may point to chronic sinus issues requiring attention. Understanding the root causes and knowing how to respond effectively can bring lasting relief and prevent complications.
Common Causes of Nasal and Sinus Burning
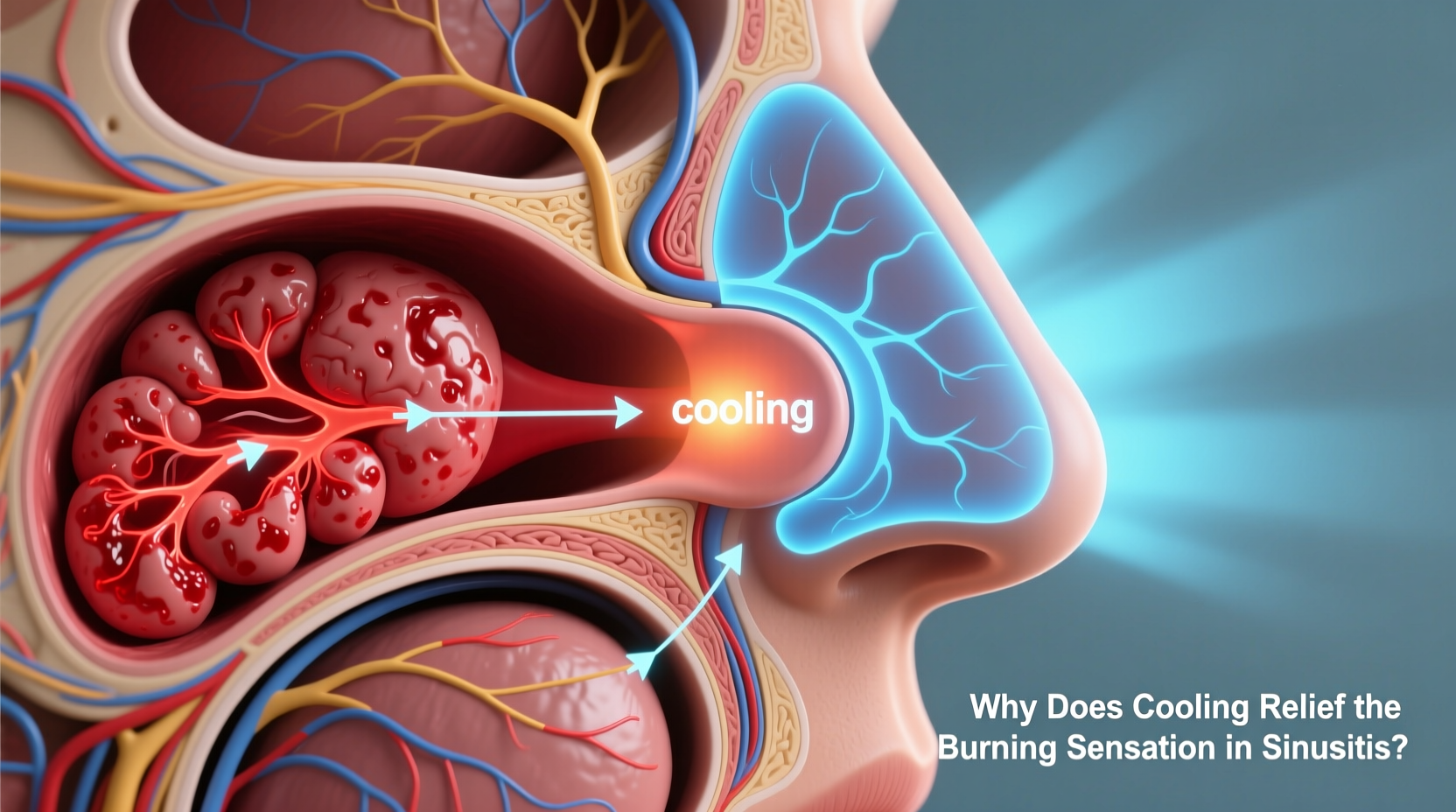
The nasal cavity is lined with sensitive tissue that reacts quickly to irritants, infections, and inflammatory conditions. When this lining becomes irritated or inflamed, it can produce a burning sensation that radiates into the forehead, cheeks, or behind the eyes—typical sinus areas.
- Allergic rhinitis: Pollen, dust mites, pet dander, and mold spores trigger immune responses that inflame nasal tissues, leading to itching, sneezing, and a burning sensation.
- Viral or bacterial sinusitis: Infections cause swelling and mucus buildup, increasing pressure and irritation in the sinuses. Acute cases last under four weeks; chronic sinusitis persists beyond 12 weeks.
- Dry air: Low humidity, especially in heated indoor environments during winter, dries out nasal membranes, making them prone to cracking and burning.
- Chemical irritants: Cleaning products, smoke, perfumes, and industrial fumes directly damage nasal tissue, causing immediate stinging.
- Nasal sprays (overuse): Decongestant sprays like oxymetazoline can cause rebound congestion and irritation when used longer than three days.
- Deviated septum or structural issues: Abnormal nasal anatomy can trap mucus and bacteria, promoting chronic inflammation and localized burning.
Medical Conditions Linked to Persistent Sinus Burning
Beyond everyday irritants, certain medical conditions contribute to ongoing nasal discomfort:
- Non-allergic rhinitis: Unlike allergies, this condition involves chronic nasal inflammation without an immune trigger. Symptoms include burning, runny nose, and postnasal drip, often worsened by weather changes or strong odors.
- Nasal polyps: Soft, noncancerous growths in the nasal passages or sinuses block airflow and drainage, creating pressure and irritation.
- Sjögren’s syndrome: An autoimmune disorder that reduces moisture production, including in the nose, leading to dryness and burning.
- GERD (gastroesophageal reflux disease): Stomach acid can travel up the throat and irritate the back of the nasal passage, contributing to a burning sensation.
“Persistent nasal burning should never be ignored—especially if accompanied by facial pain or thick discharge. It could indicate chronic sinusitis or an underlying systemic condition.” — Dr. Lena Patel, Otolaryngologist
Effective Relief Strategies for Sinus Burning
Immediate relief begins with identifying and removing triggers, followed by targeted treatments to soothe inflammation and restore moisture.
1. Humidify Your Environment
Dry air is one of the most common contributors to nasal burning. Using a cool-mist humidifier in bedrooms or workspaces adds moisture, preventing membrane dryness. Aim for 40–60% indoor humidity.
2. Saline Nasal Irrigation
Rinsing the nasal passages with sterile saline solution helps flush out allergens, mucus, and irritants. A neti pot or squeeze bottle with distilled or boiled water can reduce inflammation and provide rapid symptom relief.
3. Avoid Irritants
Limit exposure to cigarette smoke, aerosol sprays, strong perfumes, and chlorine from pools. Wearing a mask in polluted environments or while cleaning can protect sensitive nasal tissue.
4. Use Hypoallergenic Products
Switch to fragrance-free soaps, detergents, and household cleaners. These are less likely to trigger chemical irritation in the nasal passages.
5. Medicated Treatments (When Necessary)
In cases of allergy or infection, appropriate medications can resolve the root cause:
- Antihistamines for allergic reactions
- Nasal corticosteroids (e.g., fluticasone) to reduce inflammation
- Antibiotics only if bacterial sinusitis is confirmed by a doctor
Step-by-Step Guide to Soothing a Burning Nose
- Assess the environment: Check for recent exposure to smoke, chemicals, or dry air.
- Stop using nasal decongestant sprays: If used for more than three days, discontinue to avoid rebound effects.
- Perform a saline rinse: Use a pre-made saline spray or neti pot once or twice daily.
- Run a humidifier: Especially at night, to maintain moisture levels.
- Apply a thin layer of petroleum jelly: Inside the nostrils (sparingly) to protect cracked skin.
- Monitor symptoms: If burning persists beyond 7–10 days or worsens, consult a healthcare provider.
Do’s and Don’ts: Managing Sinus Burning
| Do’s | Don’ts |
|---|---|
| Use saline sprays regularly | Overuse nasal decongestants |
| Stay hydrated to thin mucus | Ignore worsening facial pain or fever |
| Wash hands frequently to prevent infection | Smoke or expose yourself to secondhand smoke |
| Keep bedroom air moist with a humidifier | Use tap water directly in neti pots |
| Track symptoms in a journal | Self-diagnose chronic sinus issues |
Real-Life Example: Chronic Burning Resolved
Sarah, a 34-year-old teacher, experienced persistent nasal burning every fall and winter. She initially attributed it to colds, but symptoms lasted months and included fatigue and pressure behind her eyes. After seeing an ENT specialist, she was diagnosed with allergic fungal sinusitis triggered by indoor mold in her classroom. With environmental controls—using an air purifier, switching to hypoallergenic cleaning supplies—and a prescription nasal steroid, her burning sensation resolved within six weeks. Her case highlights how persistent symptoms require professional evaluation rather than self-treatment.
FAQ
Can dehydration cause a burning nose?
Yes. Dehydration reduces mucus production, leaving nasal tissues dry and vulnerable to irritation. Drinking adequate water helps maintain healthy mucosal function and can alleviate mild burning sensations.
Is nasal burning a sign of COVID-19?
While not a primary symptom, some people with viral infections—including SARS-CoV-2—report nasal irritation or burning early in the illness. More common signs include fever, cough, loss of taste or smell, and fatigue. Testing is recommended if exposure is suspected.
When should I see a doctor for sinus burning?
Seek medical advice if the burning lasts more than 10 days, is accompanied by green/yellow nasal discharge, facial swelling, fever, or vision changes. These may indicate a bacterial infection or chronic sinus condition needing treatment.
Conclusion: Take Control of Your Sinus Health
A burning nose is more than just uncomfortable—it’s a signal from your body that something needs attention. Whether due to dry air, allergies, or an underlying condition, the right approach can bring fast and lasting relief. By combining environmental adjustments, proper hydration, and timely medical care, you can protect your nasal health year-round. Don’t dismiss recurring symptoms as normal. Listen to your body, act early, and consult a healthcare provider when needed.









 浙公网安备
33010002000092号
浙公网安备
33010002000092号 浙B2-20120091-4
浙B2-20120091-4
Comments
No comments yet. Why don't you start the discussion?